Recognizing Obesity as a Chronic Disease: A Policy Imperative for Canada’s Future
 Pixaby
Pixaby
By Muhammad Ilyas Nadeem, Sylvia Santosa, and Cristina Sanza
July 29, 2025
Obesity in Canada is a national health crisis that costs the country $27.6 billion annually and accounts for nearly 8% of total health care spending; numbers that underscore the urgent need for a coordinated national policy response.
Despite affecting 1 in 4 Canadians and being a known risk factor for over 200 chronic diseases, obesity itself remains unrecognized as a chronic disease in Canada. This lack of recognition has led to a fragmented and inadequate public health response nationwide — one where treatment, education, and prevention are left largely to non-governmental organizations.
There is no unified national strategy in place for how the government educates, treats, and deals with obesity. While the recent approval of weight-loss medications like semaglutide (marketed as Ozempic and Wegovy) has generated significant public interest, pharmacotherapy alone is not a substitute for a comprehensive, coordinated approach. These medications, though promising, remain inaccessible to many due to cost, limited coverage, and a lack of integrated support services such as nutritional counseling, mental health care, and long-term follow-up.
Policymakers must recognize that addressing obesity is not merely a health issue — it is a national imperative for building a healthier, more equitable, and economically sustainable Canada.
Obesity Research
Understanding obesity’s multifaceted nature is the key to developing effective treatment and prevention strategies. Biological factors, such as genetics and metabolism, play a crucial role in an individual’s likelihood of developing obesity, and suffering the consequences of this disease. Existing evidence has revealed how specific fat deposits drive these obesity-related diseases, offering pathways for targeted interventions that could reduce hospitalizations and long-term care needs. Targeting these harmful fat stores through lifestyle changes, medication, or bariatric surgery can reduce hospitalization and improve long-term outcomes.
Environmental and social factors are also important contributors. Socioeconomic status, access to healthy foods, and the built environment all influence obesity rates. More research is urgently needed to inform evidence-based policies that address these root causes.
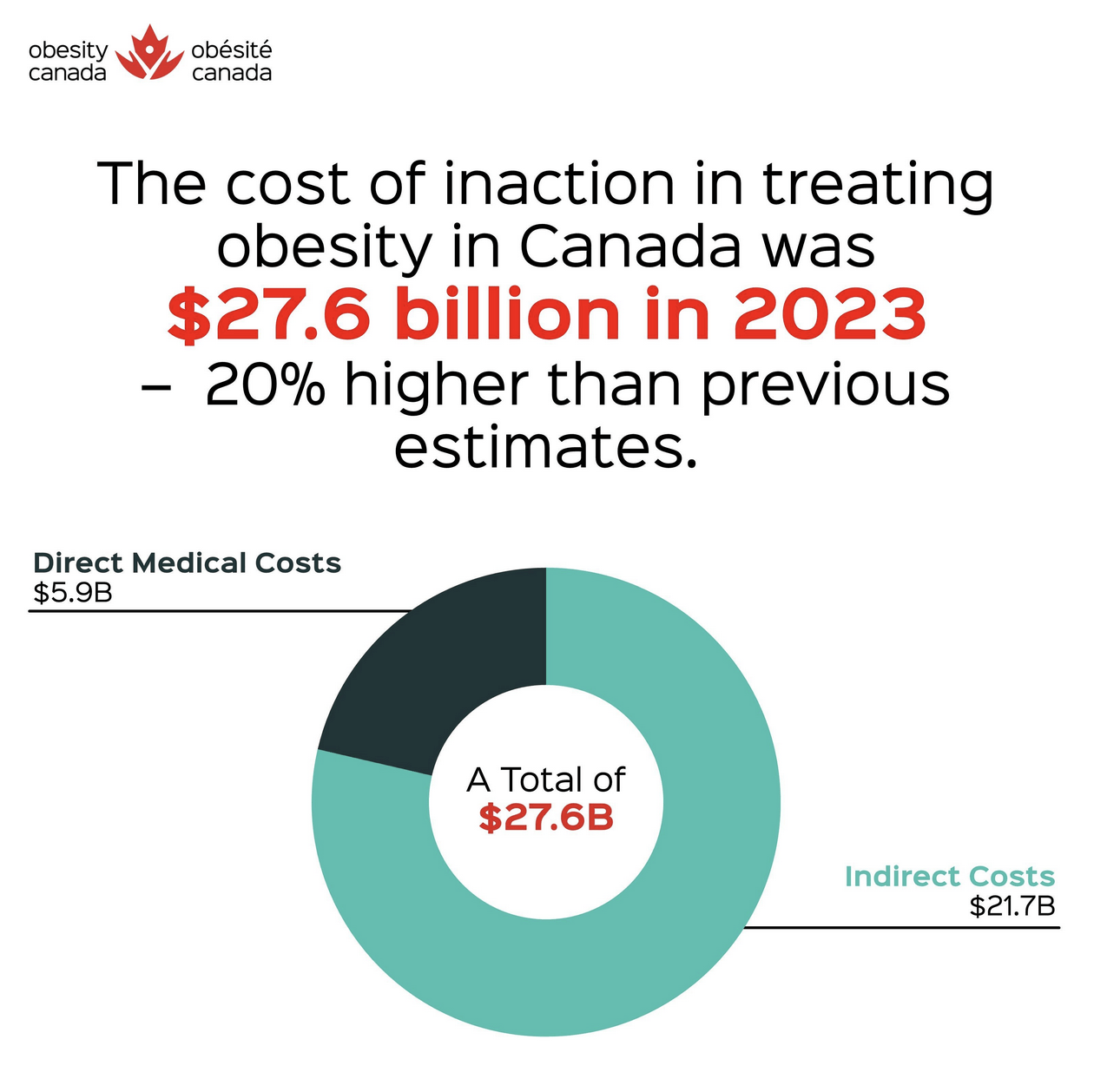
Economic Impact
Inaction in treating obesity takes an undeniable toll on Canada’s economy, reaching into the billions. Spending on obesity has increased 20% from 2021 to 2023, underscoring the urgent need for systemic intervention. Treatment of obesity-associated conditions such as type 2 diabetes, cardiovascular disease, and certain cancers adds $6 billion to health care spending. Indirectly, reduced productivity, absenteeism, and premature mortality is costing Canadians $22 billion per year. Addressing obesity proactively would alleviate the strain on health care systems and boost workforce productivity, saving billions annually.
The Price of Stigma
Despite the well-established fact that obesity stems from a range of factors beyond individual lifestyle choices, people with obesity continue to face stigma and discrimination — not only in everyday social interactions but also within health care settings. A national Canadian study found that 6.4% of adults reported experiencing discrimination in health care, with significantly higher rates among those with class II/III obesity. This stigma is linked to adverse mental health outcomes, including depression, anxiety, and avoidance of medical care.
Research also shows that internalized weight stigma can reduce adherence to treatment and worsen psychological distress. These negative societal perceptions contribute to a cycle of low self-esteem and poor health outcomes. These effects are especially pronounced among Indigenous and racialized communities, who face systemic barriers to care, including food insecurity, limited access to physical activity resources, and culturally insensitive health care practice, making obesity a critical issue of social justice.
Public education campaigns, equitable access to treatment, and culturally informed care are essential to dismantle stigma and promote healthier outcomes for all Canadians.
Recognizing Obesity as a Chronic Disease
In March 2025, Alberta became the first province in Canada to officially recognize obesity as a chronic disease. This landmark move aims to reduce weight bias, improve access to treatments such as pharmacotherapy and bariatric surgery, and integrate obesity care into the broader health care system.
While care models and access to obesity medications are evolving, most provinces continue to unjustly frame obesity primarily as a lifestyle issue. The lack of recognition of obesity as a chronic disease limits access to comprehensive, evidence-based care. Almost every Canadian is directly or indirectly affected by obesity, yet fewer than 20% of Canadians with private drug plans have coverage for obesity medications and wait times for bariatric surgery can exceed eight years, especially in rural areas. Expanding coverage and training more obesity specialists are essential to improving access.
Research and education are essential to effective obesity care —especially in challenging the myth that obesity is a personal failing. Although the Canadian Adult Obesity Clinical Practice Guidelines developed by Obesity Canada and the Canadian Association of Bariatric Physicians and Surgeons offer a comprehensive, evidence-based framework for patient-centered care, they are not yet part of a federal policy strategy.
These guidelines emphasize reducing weight bias, addressing biological and social determinants of obesity, and supporting long-term, individualized care through interventions such as behavioral therapy, pharmacotherapy, and surgery. Policymakers should adopt and integrate these guidelines into national and provincial health systems to ensure equitable prevention strategies and personalized, science-based care.
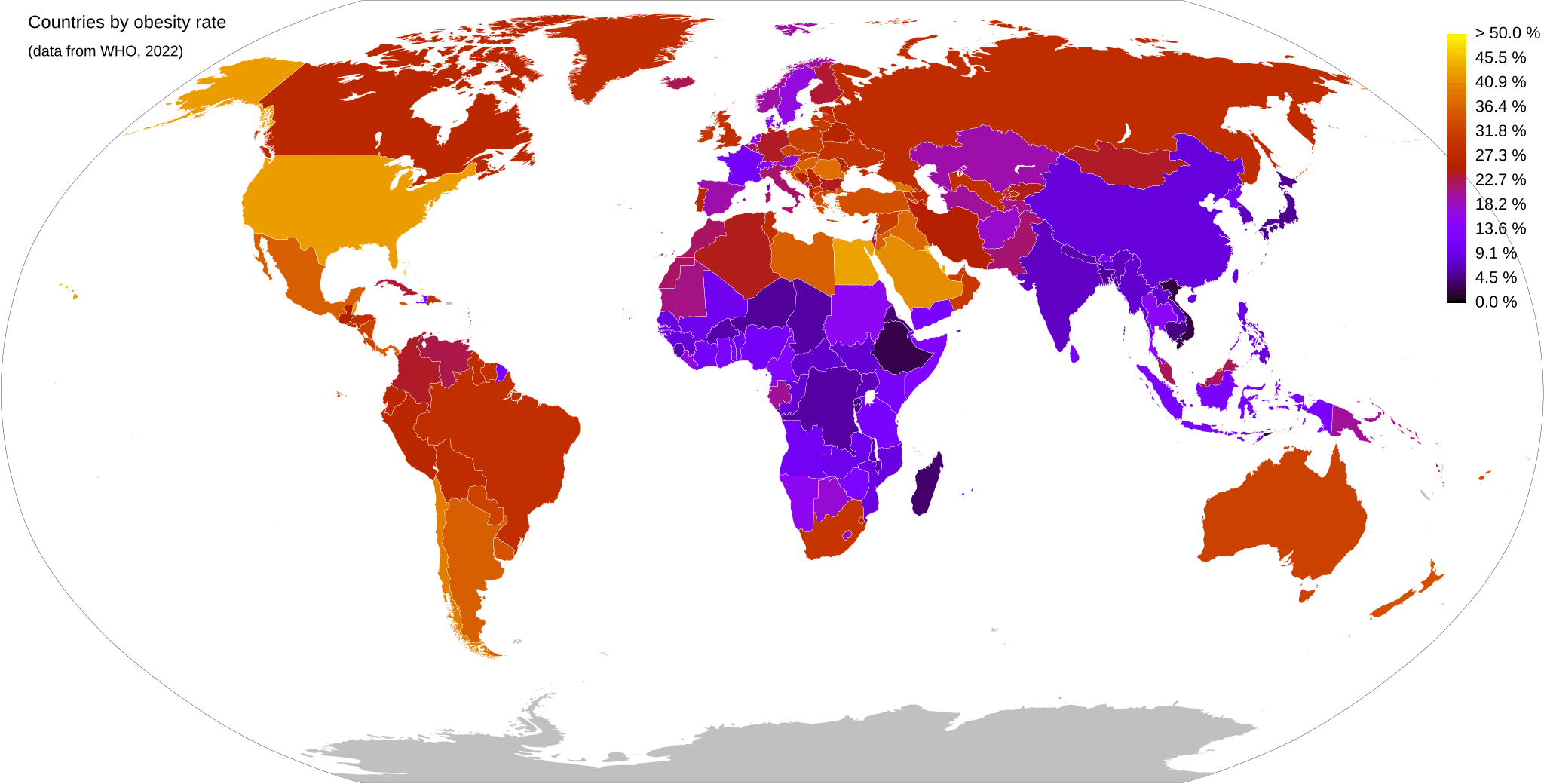
Global Best Practices
Several countries have emerged as leaders in addressing obesity through coordinated, multisectoral policies and comprehensive public health strategies. In France, strict regulations on food advertising to children and a soda tax have contributed to healthier consumption patterns. Brazil has implemented a nationally coordinated school meal program that prioritizes fresh, local foods and nutrition education. Meanwhile, Chile has introduced front-of-package warning labels and marketing restrictions on unhealthy foods, leading to measurable declines in sugary drink consumption. These examples demonstrate how multisectoral, prevention-focused policies can effectively reduce obesity rates and promote long-term health outcomes.
Immediate Action
The time for action is now. Canada’s policymakers must adopt a coordinated, population-level strategy to address obesity — just as they have done for dementia and diabetes. The National Dementia Strategy emphasizes prevention, equity, and quality of life through multi-sector collaboration, while the Framework for Diabetes in Canada outlines a unified approach to prevention, treatment, and research across all levels of government. As a leading driver of chronic diseases, including Alzheimer’s and diabetes, obesity deserves the same strategic focus.
To effectively address obesity and improve society, decision-makers should take four key steps:
- Recognize obesity as a chronic disease across all provinces — to unlock funding, reduce stigma in health care, and improve access to proven treatments.
- Invest in research — studying both biological and social factors to develop better prevention and treatment strategies would ensure inclusive, effective solutions.
- Address systemic inequities — national public education campaigns and education for health care workers are needed to reduce stigma, emphasize workplace wellness programs, raise awareness about obesity’s complexity, and promote equitable and supportive environments for prevention and treatment.
- Strengthening the public health care system – improving access to primary care, expanding drug coverage and addressing racism in health care settings.
Obesity is not a personal failure — it’s a public health challenge that demands coordinated, evidence-based action. By recognizing obesity as the disease that it is, prioritizing research, and addressing systemic inequalities to optimize prevention and equitable care, Canada can reduce the health and economic cost of obesity and build a healthier, more inclusive future for all.
Muhammad Ilyas is a doctoral candidate in Health and Exercise Science at Concordia University. His research explores regional variations in fat tissue, inflammation, and weight loss responses in obesity and Type 2 Diabetes. He advocates for evidence-based policies that address obesity’s complexity and promote equitable health outcomes for all Canadians.
Sylvia Santosa, Ph.D., R.D., is a Canada Research Chair in Clinical Nutrition and Professor at Concordia University. Her research explores how fat tissue from different body regions affects obesity and metabolic disease, advancing personalized treatment approaches. She advocates for science-informed policies that address obesity’s complexity and promote healthier aging for Canadians.
Cristina Sanza is a Digital Journalism Instructor at Concordia University and a researcher at the Centre for Journalism Experimentation. Her work explores innovative ways to engage the public in science and health through fitness media. She also coordinates Concordia’s international science journalism summer school, Projected Futures.
